Mark Easley, MD
Duke Health
I have had the distinct privilege serving on the Exactech total ankle design team with three other surgeons, my Duke University partners Jim DeOrio, MD and Jim Nunley, MD and our Swiss colleague, Victor Valderrabano, MD. Over the past 25 years we have had extensive experience with most every major total ankle system, including fixed- and mobile-bearing designs. Jim, Jim and Victor are unequivocally international thought leaders in total ankle arthroplasty (TAA). As a group, arguably we have unparalleled clinical and research experience with TAA.1-5 Each of us has formulated potential improvements to the existing body of knowledge of TAA and has had some hand in the improvement of existing total ankle systems or development of potential new systems. Roughly five years ago, we realized that our collective efforts would be far more effective.
Exactech offered the perfect opportunity for the four of us to optimize our contributions to optimal treatment of patients with end-stage ankle arthritis. The Exactech team of Matt Hamilton, PhD (Manager of Lower Extremity Engineering), Steve Norton (Product Development Engineer), Medhut Alnadi (Product Design Engineer), Phong Diep (Sr. Designer), Emery Patton (Director of Marketing), and Rick Andrews (Sr. Product Manager), with its experience in Exactech’s other joint arthroplasty systems, provided us with the engineering and implant development expertise needed to convert our visions into a superior and practical total ankle implant. The combination of our surgical experience and the Exactech’s team’s talent for implant development proved to be ideal.
The Vantage® Total Ankle System incorporates numerous features favored in currently used total ankle designs while introducing several new ones. What especially stands out for the Vantage is that rather than use imaging or cadaver specimens of physiologic normal ankles, 73 CT scans of arthritic ankles served as the template to optimize the tibial and talar implant backside designs.6 The Vantage is available in both fixed- and mobile-bearing designs. The fixed-bearing implant is cleared for sale in the United States, and the mobile-bearing implant is cleared for sale in Europe, as of this writing.

The Vantage tibial component maximizes the contact area on the prepared tibial plafond surface, featuring a recessed area to accommodate the fibula while maximizing tibial component cortical support. (Figure 1) To diminish joint fluid gaining access to the tibial component’s backside and creating component loosening, recent trends in TAA technique favor not violating the anterior tibial cortex.
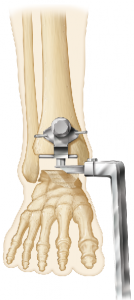
(Figure 2) The Vantage’s technique confers the advantage of vertically oriented tibial component fixation in contrast to most other modern systems that utilize obliquely orientated tibial pegs to avoid violating the anterior tibial cortex or traditional horizontally oriented tibial fixation that require anterior tibial cortex penetration.
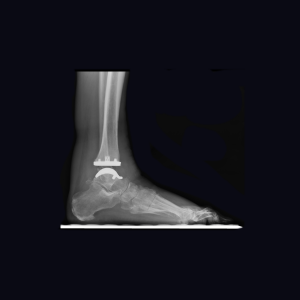
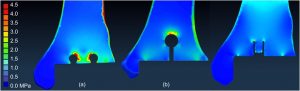
(Figure 3) Finite element modeling suggests that vertically oriented pegs provide ideal loading characteristics on the tibial bone-implant interface, thereby diminishing the risk of eccentric stresses, stress shielding and the chance of tibial component loosening.
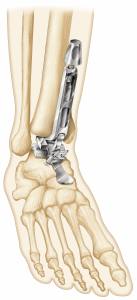
(Figure 4) Moreover, the Vantage tibial component’s central cage, similar to the cage featured on the Exactech reverse total shoulder system, affords not only reliable press-fit fixation but adds the potential for bone ingrowth and superior long-term fixation.
 |
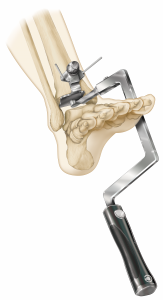 |
(Figure 5) The instrumentation to prepare the tibia for vertical peg and cage orientation is unique and simple to use (Figure 6); the Exactech engineering team was brilliant in creating this impaction system disproving many doubters, including myself, that such an impactor could be safely introduced despite the ankle joint’s relatively limited access. The Vantage talar component’s backside has a uniform curve that optimizes compressive forces on the prepared dome-shaped talus throughout the ankle’s full range of motion. In contrast, nearly all competitors’ talar components provide alarm component stability via chamfer cuts that tend to create the potential for shear stresses. (Figure 5) One recently released total ankle system, features a uniform dome-shaped talar preparation like that of the Vantage but requires a lateral approach and fibular osteotomy for component implantation. The Vantage’ talar component confers the same talar component advantages via the far more commonly used anterior approach and does not require a fibular osteotomy. Unique to the Vantage total ankle system, a simple manual rasp is used to complete the uniform talar dome preparation.
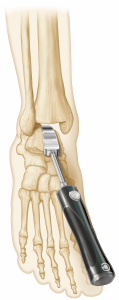
(Figure 7) Two anterior pegs designed to provide initial component stability do not detract from the uniformly compressive forces throughout the range of motion. The central talar component sulcus on the components articulating surface maintains the Vantage’s coronal plane stability for the polyethylene and ankle.
Based on the successful Exactech total knee polyethylene implant, the Vantage’s polyethylene component, affords high fracture toughness and low wear rates. The polyethylene, with its congruent articulation on the talar component, affords satisfactory coronal plane ankle stability without creating undue constraint. (Figure 2) Unique to the Vantage fixed-bearing total ankle system is the locking clip technology that secures the polyethylene to the tibial tray. (Figure 8) Through exhaustive stress and cyclic load testing, the Vantage team of engineers confirmed that the locking clip maintains satisfactory polyethylene fixation to the tibial tray; yet, extraction is easy should the polyethylene need to be exchanged.
 |
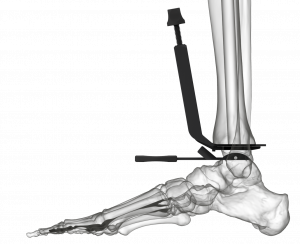 |
Our ankle design team spent the better part of four years devising and perfecting the Vantage surgical technique. Our initial thoughts favored sophistication and complexity to confer advantages over the competitors’ ankles. However, complexity and its accompanying frustrations soon gave way to simplicity. The current surgical technique and instrumentation is remarkably straightforward. I recently taught a Vantage cadaver lab to a group of residents; none of the residents had prior experience performing a total ankle replacement. I can confidently state that the residents’ implanted Vantage ankles were on par with the first Vantage cadaveric ankle implantations of nearly every experienced foot and ankle surgeon at our training labs. The external tibial alignment guide is reliable in properly orienting the tibial cut, and punching the relief areas for the tibial component pegs and cage is easily learned. Talar preparation is uncomplicated, with reproducible positioning of the talar component in both the coronal and sagittal planes (Figure 9); creating the uniform talar dome arc is facilitated by the user-friendly manual rasp.
September 30, 2017 was the one-year anniversary of the first Vantage total ankle implantation, a fixed-bearing ankle that Dr. Nunley and I performed at Duke University Medical Center. Since then my Duke colleagues and I have performed more than 100 Vantage total ankles, have trained numerous foot and ankle specialists throughout the United States and have seen the first wave of successful Vantage implantations by a talented group of surgeons that now favor the Vantage for treating end-stage ankle arthritis. Dr. Valderrabano will soon begin implanting the mobile-bearing Vantage in Switzerland and train many European foot and ankle specialists.
locking clip technology that secures the polyethylene to the tibial tray.
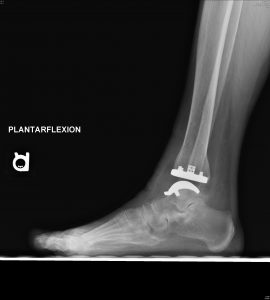
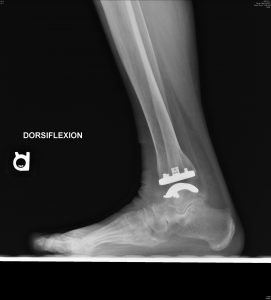
Follow-up is too short at this point to report outcomes for the Vantage. However, my colleagues and I have been collecting data on every Vantage that we implant, including validated patient-reported outcomes, accepted objective outcomes measures and standardized radiographic evaluations. (Fig 10 A and B) To date, our observations reflect high patient satisfaction, low complication rates and a trend toward favorable range of motion confirmed with objective postoperative radiographic dorsiflexion and plantarflexion measurements. While my colleagues and I initially limited the Vantage to end-stage ankle arthritis with minimal deformity, more recently we expanded indications to include varus and valgus ankle arthritis. At early follow-up our results are equally favorable for end-stage ankle arthritis with and without deformity.
The future of the Vantage is, in my mind, rather bright. Within the next six months the Exactech team of engineers anticipates completion of a dome-replacing “flat top” talus that will allow surgeons to safely perform TAA for ankle arthritis associated with talar dome cysts, focal AVN, and extensive talar dome wear.* The dome-replacing talar component will also be used in revision TAA.* We have also begun designing an augmented tibial component for ankle arthritis associated with a deficient distal tibia or for revision surgery. Although some competitors have similar augmented or revision components, they lack the advantages of the Vantage total ankle design. Computer-assisted orthopaedic surgery and patient-specific options for the Vantage are planned. Drs. DeOrio, Nunley, Valderrabano and I look forward to the continued success working with Exactech’s ankle design team.
References
1.Stewart MG, Green CL, Adams SB Jr, DeOrio JK, Easley ME, Nunley JA. Midterm Results of the Salto Talaris Total Ankle Arthroplasty. Foot Ankle Int. 2017 Jul 1:1071100717719756. doi: 10.1177/1071100717719756. [Epub ahead of print]
2. Adams SB Jr, Demetracopoulos CA, Queen RM, Easley ME, DeOrio JK, Nunley JA. Early to mid-term results of fixed-bearing total ankle arthroplasty with a modular intramedullary tibial component. J Bone Joint Surg Am. 2014 Dec 3;96(23):1983-9. doi: 10.2106/JBJS.M.01386.
3. Queen RM, Sparling TL, Butler RJ, Adams SB Jr, DeOrio JK, Easley ME, Nunley JA. Patient-Reported Outcomes, Function, and Gait Mechanics After Fixed and Mobile-Bearing Total Ankle Replacement. J Bone Joint Surg Am. 2014 Jun 18;96(12):987-993. 4. Nunley JA, Caputo AM, Easley ME, Cook C. Intermediate to long-term outcomes of the STAR Total Ankle Replacement: the patient perspective. J Bone Joint Surg Am. 2012 Jan 4;94(1):43-8. doi: 10.2106/JBJS.J.01613.
5. Brunner S, Barg A, Knupp M, Zwicky L, Kapron AL, Valderrabano V, Hintermann B. The Scandinavian total ankle replacement: long-term, eleven to fifteen-year, survivorship analysis of the prosthesis in seventytwo consecutive patients. J Bone Joint Surg Am. 2013 Apr 17;95(8):711-8. doi: 10.2106/JBJS.K.01580.
6. Wiewiorski M, Hoechel S, Anderson AE, Nowakowski AM, DeOrio JK, Easley ME, Nunley JA, Valderrabano V, Barg A. Computed Tomographic Evaluation of Joint Geometry in Patients With End-
Stage Ankle Osteoarthritis. Foot Ankle Int. 2016 Jun;37(6):644-51. doi: 10.1177/1071100716629777. Epub 2016 Feb 3.
